The Procedure
About The Vasectomy Reversal Surgery
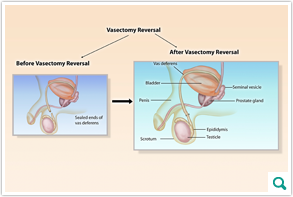 A vasectomy reversal is a microsurgical procedure to restore the connection
of the vas deferens that were previously cut during a vasectomy. The vas
deferens is the tube that carries sperm to the ejaculate. Our microsurgeons
are experienced in both the
vasovasostomy surgery and in the more delicate microsurgery called
epididymovasostomy.
A vasectomy reversal is a microsurgical procedure to restore the connection
of the vas deferens that were previously cut during a vasectomy. The vas
deferens is the tube that carries sperm to the ejaculate. Our microsurgeons
are experienced in both the
vasovasostomy surgery and in the more delicate microsurgery called
epididymovasostomy.
Both procedures require microsurgery. The channel of the vas deferens through which the sperm swim is only .3 to .4 millimeters in diameter. Therefore, it is necessary to use a state-of-the-art microscope that provides 16 times the magnification of the operating image. The training and precise skills of the surgeon are of the utmost importance.
Sperm are produced in the testis. They are stored and reach maturation in the epididymis, a tightly coiled, muscular tube that is 15 to 18 feet long and leads into the vas deferens. The muscle of the epididymis contracts to propel the sperm through the vas deferens and into the urethra at the far end of the penis so the sperm can fertilize an egg.
The decision to perform a vasovasostomy or an epididymovasostomy depends upon the quality of the fluid contained in the testicular side of the vas deferens. To check this, the surgeon expresses the fluid during surgery and examines it under a microscope.
Once The Sperm Is Analyzed, There Are Three Possibilities:
- If sperm are present in the fluid, a vasovasostomy connecting the two severed ends of the vas can be performed. The success rate for this type of patient is up to 95 percent for a return of sperm to the ejaculate.
- If no sperm are present in the fluid, but the vasal fluid is abundant, clear, and watery, then the right conditions are present for sperm production, and the vasovasostomy can still be performed.
- However, when the fluid is thick and pasty, which indicates poor quality, and if sperm is absent or there is no fluid at all, this means there is a blockage that requires an epididymovasostomy. Instead of connecting the two ends of the vas deferens, the surgeon will connect the end of the vas deferens to the epididymis. Approximately 50 percent of men have a return of sperm to their ejaculate following an epididymovasostomy.
